Why Changing Weather Makes Rheumatoid Arthritis Worse: The Hidden Link Between Climate and Joint Pain
Many people living with Rheumatoid Arthritis (RA) notice that their symptoms fluctuate throughout the year. Some patients report increased joint stiffness during winter mornings, while others experience flare-ups during humid or rainy weather.
This observation is not just anecdotal. Increasing scientific evidence suggests that environmental factors such as temperature, humidity, atmospheric pressure, and seasonal variation can influence inflammation levels in autoimmune diseases like rheumatoid arthritis.
Understanding how climate and environmental changes affect RA can help patients manage symptoms more effectively and reduce flare-ups.
Understanding Rheumatoid Arthritis
Rheumatoid arthritis is a chronic autoimmune disease in which the immune system mistakenly attacks the lining of joints (synovium). This leads to inflammation, swelling, stiffness, and progressive joint damage.

Unlike osteoarthritis, which results from wear and tear, RA is driven by immune system dysregulation and systemic inflammation.
Symptoms often include:
- Morning joint stiffness
- Joint swelling and tenderness
- Fatigue
- Reduced mobility
- Symmetrical joint involvement
How Environmental Changes Influence Rheumatoid Arthritis
Environmental conditions can influence pain perception, inflammatory pathways, and joint tissue behavior. These changes may not cause rheumatoid arthritis directly, but they can significantly affect symptom severity.
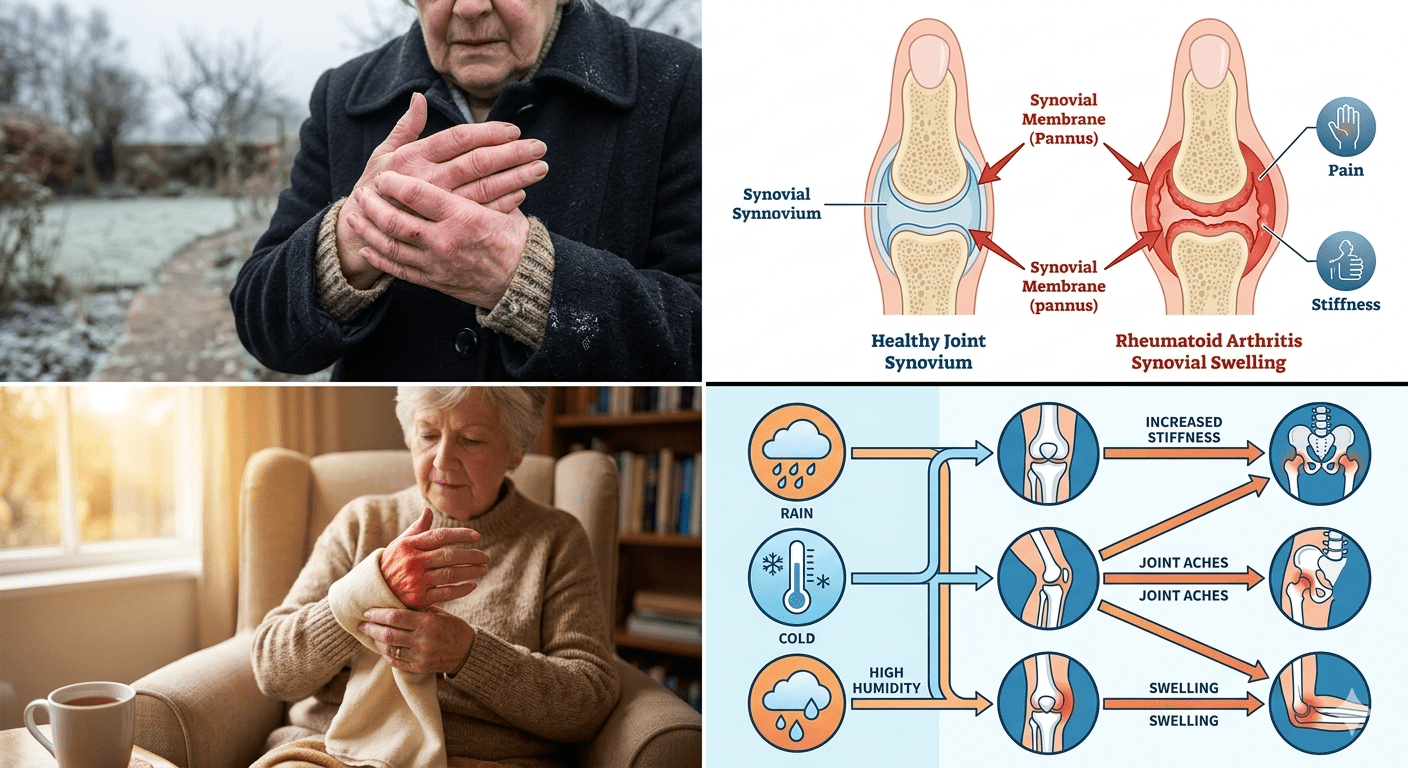
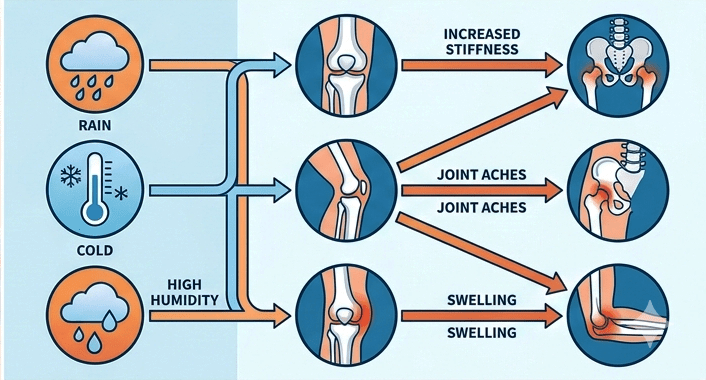
1. Temperature Changes
Cold temperatures can cause muscles, ligaments, and joint tissues to tighten. In people with RA, this stiffness can increase pain and reduce joint mobility.
Cold weather may also slow circulation, which can intensify inflammation in already affected joints.
2. Humidity and Damp Weather
High humidity levels may increase joint swelling. Damp conditions can affect joint capsule pressure and nerve sensitivity, leading to increased pain perception.
Many RA patients report worsening symptoms before rainy weather due to atmospheric pressure changes.
3. Barometric Pressure Changes
Barometric pressure refers to the weight of the air in the atmosphere. When pressure drops before storms or weather shifts, tissues around joints may expand slightly, irritating surrounding nerves.
This phenomenon may contribute to the commonly reported “weather pain” in arthritis.
4. Seasonal Variations
Seasonal shifts may influence immune system activity. During winter, reduced sunlight exposure leads to lower vitamin D levels, which may worsen inflammatory processes in autoimmune diseases.
Seasonal infections and reduced physical activity may also trigger RA flare-ups.
5. Climate Change and Autoimmune Diseases
Emerging research suggests that global climate change may influence autoimmune disease patterns through increased environmental stressors, air pollution, and infectious triggers.
While research is ongoing, scientists believe environmental stress can alter immune responses and inflammatory pathways.
Scientific Reasons Behind Climate-Related RA Flare Ups
Several biological mechanisms explain why environmental changes influence rheumatoid arthritis severity.
- Changes in inflammatory cytokine activity
- Altered nerve pain sensitivity
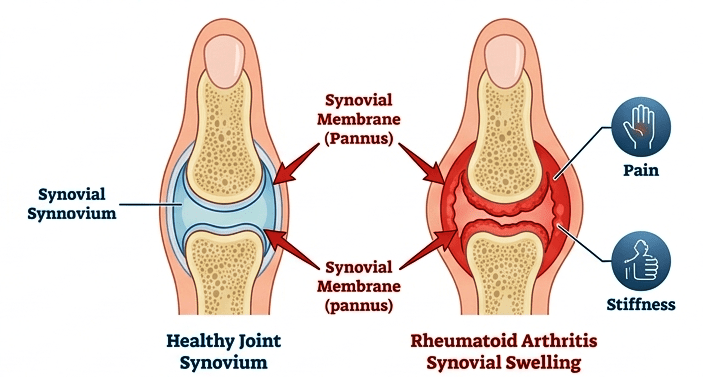
nflammation of synovial joints is the key mechanism behind RA pain. - Reduced vitamin D synthesis
- Changes in joint fluid viscosity
- Stress hormone fluctuations
These physiological responses may increase joint inflammation and pain sensitivity during weather changes.
Real-Life Example
A 45-year-old patient with long-standing rheumatoid arthritis reported increased joint stiffness every winter. Laboratory tests remained stable, but symptom severity worsened during cold months.
After introducing daily light exercise, vitamin D supplementation, and thermal joint protection strategies, seasonal flare-ups significantly reduced.
How Patients Can Manage Weather-Related RA Symptoms
Stay Physically Active
Gentle exercises such as walking, stretching, yoga, and physiotherapy help maintain joint flexibility and reduce stiffness.
Maintain Body Warmth
Wearing thermal clothing and using warm compresses can reduce joint stiffness during cold weather.
Optimize Vitamin D Levels
Sunlight exposure and vitamin D supplementation may support immune regulation.
Monitor Weather Patterns
Tracking symptom changes with weather patterns may help anticipate flare-ups.
Follow Medical Treatment
Regular use of disease-modifying antirheumatic drugs (DMARDs) prescribed by physicians remains essential.
Doctor’s Insight
Doctor’s Insight: While weather changes alone do not cause rheumatoid arthritis, environmental factors can significantly influence symptom severity. Patients should focus on maintaining joint mobility, avoiding prolonged cold exposure, and continuing disease-modifying therapy. Early management of flare-ups helps prevent long-term joint damage.
Frequently Asked Questions (FAQ)
Does cold weather worsen rheumatoid arthritis?
Cold temperatures can increase joint stiffness and reduce mobility, which may worsen pain in RA patients.
Why do joints hurt before rain?
Changes in barometric pressure may cause joint tissues to expand slightly, increasing nerve sensitivity.
Is humidity bad for rheumatoid arthritis?
High humidity may worsen joint swelling and discomfort in some patients.
Does sunlight help rheumatoid arthritis?
Sunlight helps the body produce vitamin D, which plays an important role in immune regulation and inflammation control.
Can climate change affect autoimmune diseases?
Some researchers believe environmental changes may influence immune system behavior and inflammation patterns.
—
Summary
- Environmental changes can influence rheumatoid arthritis symptoms.
- Cold temperatures increase joint stiffness.
- Humidity and pressure changes may trigger pain.
- Vitamin D deficiency during winter may worsen inflammation.
- Regular exercise and proper treatment help manage symptoms.
Medical Disclaimer
Disclaimer: This content is provided for general informational and educational purposes only and does not constitute medical advice, diagnosis, or treatment. The information presented is not intended to replace consultation with a qualified healthcare professional, physician, or rheumatologist. While efforts are made to ensure the accuracy and reliability of the information, no guarantees are made regarding completeness, timeliness, or medical applicability. The authors, publishers, and affiliated organisations disclaim any liability for decisions made based on this content. Rheumatoid arthritis and related symptoms can vary widely among individuals, and environmental influences such as weather or climate should not be considered a sole basis for medical decisions or treatment changes. Users are advised to seek professional medical guidance before making any healthcare decisions, including medication changes, lifestyle modifications, or treatment plans. Limitation of Liability: Under no circumstances shall the authors, website, or publishers be liable for any direct, indirect, incidental, or consequential damages arising from the use or misuse of this information. No Doctor-Patient Relationship: Use of this content does not establish a doctor-patient relationship. Emergency Notice: If you are experiencing a medical emergency, severe symptoms, or acute worsening of your condition, seek immediate medical attention or contact your local emergency services.